Allergic eye disease is a bilateral immune mediated process of the ocular surface that occurs in up to 25% of the population of developed countries. Five entities are described as having at least in part some portion of their pathogenesis emanating from mast cell activation: Allergic Conjunctivitis, as seasonal (SAC), or Perennial Allergic Conjunctivitis (PAC), Atopic Keratoconjunctivitis (AKC), Vernal Keratoconjunctivitis (VKC), and Giant Papillary Conjunctivitis (GPC). SAC, PAC, and GPC are non-vision threatening where as AKC and VKC may lead to vision loss. The severe forms of allergic disease, AKC and VKC have an immune mediated pathogenesis as well as mast cell activation. GPC is considered iatrogenic due to the presence of an ocular surface foreign body such as contact lens or an exposed suture. Treatment of allergic eye disease may be as simple as administration of artificial tears or topical antihistamines through to as complex as the need for topical or oral steroids as well as immunomodulatory therapy. Contact dermatitis may occur in the periocular region. The periocular form of contact dermatitis is most commonly associated with topical ophthalmic pharmaceutical agents. Antiviral and glaucoma medications are some of the more common medications implicated. In-vivo conjunctival provocation testing is an ocular equivalent of skin testing to determine sensitivity to specific antigens. This may be used experimentally to develop a reproducible human model of allergic eye disease and has been utilized to test new pharmaceutical agents. This article focuses on Allergic Conjunctivitis.
Allergic Conjunctivitis – Seasonal/Perennial
Introduction
Allergic conjunctivitis (AC) is a bilateral, self-limiting conjunctival inflammatory process. It occurs in sensitized individuals (no gender difference) and is initiated by allergen binding to IgE antibody on resident mast cells contained within the conjunctiva. The importance of this process is related more to its frequency rather than its severity of symptoms. The two forms of AC are defined by whether the inflammation and symptoms occur seasonally (spring, fall) or perennially (year-round). While the inflammatory signs and symptoms are similar for both entities, seasonal allergic conjunctivitis (“hay fever conjunctivitis”) is more common. It accounts for the majority of cases of AC and is related to pollens (e.g. grass, trees, ragweed) that appear during specific seasons. Perennial allergic conjunctivitis is often related to animal dander, dust mites, or other allergens that are present in the environment year-round. Both SAC and PAC must be differentiated from the sight-threatening allergic diseases of the eye, namely AKC and VKC.
Historical Perspective
Hypersensitivity reaction description of the ocular surface dates to the earliest descriptions of hayfever or rhinitis. Some of the earliest allergy provocation testing was performed in the conjunctiva.
Epidemiology
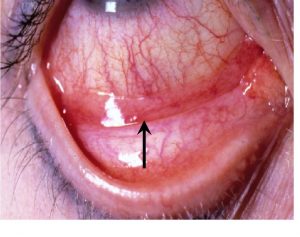
Prevalence estimates for allergic conjunctivitis are difficult because allergies in general tend to be considerably underreported. As high as 40% of the population may suffer from symptoms of allergic conjunctivitis. Importantly, 46% of all allergic conjunctivitis sufferers have associated allergic rhinitis. The distribution of SAC depends largely on the climate. For example, in the United States grass pollen – induced SAC generally occurs in the Gulf Coast and southwestern areas of the country from March to October and from May to August, in most of the rest of the country. Conversely, ragweed pollen – induced SAC occurs in most of the country during August through October, but in the southern-most states it can begin as early as July and stretch out through November. Tree pollens can become a problem as early as January in the south, and March in the north. Race and gender predilection follows that of rhinitis sufferers. Clinical Features (Figure 1) The dominant symptom reported in allergic conjunctivitis is ocular itching (Table 1). Itching can range from mild to severe. Other symptoms include tearing (watery discharge), redness, swelling, burning, a sensation of fullness in the eyes or eyelids, an urge to rub the eyes, sensitivity to light, and occasionally blurred vision. As stated previously, allergic conjunctivitis is often associated with symptoms of allergic rhinitis. Conjunctival hyperemia and chemosis with palpebral edema are typical. A rapid test for tear IgE level has correlated the objective sign of giant papillae with the total IgE tear level. (Mimura et al. 2012) Hyperemia is the result of vascular dilatation while edema (chemosis) occurs because of altered permeability of post-capillary venules. “Allergic shiners” (periorbital darkening), due to an increase of periorbital pigmentation resulting from the decreased venous return in the skin and subcutaneous tissue, are also common.
Patient evaluation, diagnosis, and differential diagnosis
An individual suspected of having allergic conjunctivitis should have a thorough ocular, medical and medication history. This will help greatly in differentiating AC from other ocular processes (Table 1). This history should establish whether the process is acute, subacute, chronic or recurrent. It should further delineate whether the symptoms/signs are unilateral or bilateral, and whether they are associated with any specific environmental or work-related exposure. Ocular symptoms such as tearing, irritation, stinging and burning are nonspecific. A history of significant ocular itching and a personal or family history of “hay fever”, allergic rhinitis, asthma or atopic dermatitis are suggestive of ocular allergy. Because AC is secondary to environmental allergens as opposed to transmission by eye-hand contact (infectious etiology), unless occurring in the context of petting an animal then rubbing one’s eye, SAC and PAC usually present with bilateral symptoms. This is in contrast to transmissible infections caused by viruses and bacteria that in general initially present in one eye, with the second eye becoming involved a few days later. Itch is an uncommon complaint during infectious conjunctivitis episodes. Furthermore, viral conjunctivitis may cause subepithelial corneal infiltrates not seen in AC. Palpable pre-auricular nodes would also signify infectious etiology for the ocular symptoms.
The type of ocular discharge, (watery, mucoid, or grossly purulent), can also be helpful in determining the underlying cause of conjunctival inflammation. A watery discharge is most commonly associated with viral or allergic ocular conditions. A mucoid or purulent discharge, with morning crusting and difficulty opening the eyelids, would strongly suggest a bacterial infection. In allergic inflammation, the eye appears red. Vision, pupil shape, ocular movement, light reactivity, and the red retinal reflex remain normal in allergic conjunctivitis. Dry eye (secondary to a decrease of the aqueous portion of the tear film) gives symptoms suggestive of foreign body in the eye and may result in conjunctiva redness. Similar symptoms are possible from anticholinergic side effects of systemic medications. Typically, itch is not reported with dry eye. Medication history should include questions concerning the patient’s use of over-the-counter topical ocular medications, cosmetics, contact lenses, and systemic medications. Any of these can produce acute or chronic conjunctivitis. This inquiry should include direct questions and should not rely on the patient to volunteer information. Many individuals do not appreciate the potential for nonprescription topical ocular medications to cause eye symptoms or partially treat AC. Differentiation of AC from the more chronic and sight threatening forms of allergic eye disease is discussed below in the context of the specific conditions.
Treatment
Medications approved for use in allergic eye disease are found in Table 2. Allergic conjunctivitis can be debilitating and may cause the individuals affected to seek any type of help for relief of symptoms. Itching and tearing may be unbearable and sleepless nights frequent. Allergic conjunctivitis symptoms may be worse than the nasal symptoms in those suffering from rhinoconjunctivitis. Furthermore, treatment of the nasal symptoms with topical nasal steroids may help the rhinitis, but not be effective for relieving ocular symptoms. Management of allergic conjunctivitis is, therefore, primarily aimed at alleviating symptoms. The best treatment is avoidance of the specific allergen, which, unfortunately, is usually not possible. Avoidance of scratching or rubbing, application of cool compresses, artificial tears and refrigeration of topical ocular medications are practical interventions to alleviate discomfort. While oral antihistamines may help to relieve eye itch, first generation drugs may also decrease tear production, causing more ocular symptoms. Topical medications are generally considered more effective to relieve ocular itching than oral medications and may be additive to relief gained from oral antihistamines. The treatment of choice for mild to moderate AC is a dual acting topical ocular medication. The mast cell stabilizing component of these drugs benefits patients most if treatment is started before the height of symptom onset. Patients usually note rapid onset of relief of itch upon drop instillation, as most dual action medications have high H1 receptor affinity. Drug dosing varies from one to four times per day and efficacy is judged best by symptom relief.
In summary, Allergic conjunctivitis is a bilateral allergic response of the conjunctiva to airborne allergens to which an individual is sensitized. The symptoms may be seasonal or year round, the signs mild without threat to vision, and the treatment with topical antihistamine drops quite effective as treatment. Loss of vision from the disease would be rare.
Table 1: Allergic Diseases of the Eye:
Disease |
Clinical Parameters |
Signs/Symptoms |
Differential Diagnosis |
| Seasonal Allergic Conjunctivitis (SAC) | Sensitized individuals Both females and males Bilateral involvement Seasonal allergens Self limiting |
Ocular itching Tearing (watery discharge) Chemosis, redness Often associated with rhinitis Not sight threatening |
Infective Conjunctivitis Preservative Toxicity Medicamentosa Dry Eye PAC/AKC/VKC |
| Perennial Allergic Conjunctivitis (PAC) | Sensitized individuals Both females and males Bilateral involvement Year-round allergens Self limiting |
Ocular itching Tearing (watery discharge) Chemosis, redness Often associated with rhinitis Not sight threatening |
Infective Conjunctivitis Preservative Toxicity Medicamentosa Dry Eye SAC/AKC/VKC |
| Atopic Keratoconjunctivitis (AKC) | Sensitized individuals Peak incidence 20-50 years of age Both females and males Bilateral involvement Seasonal/Perennial Allergens Atopic Dermatitis Chronic symptoms |
Severe ocular itching Red flaking periocular skin Mucoid discharge, photophobia Corneal erosions Scaring of conjunctiva Cataract (anterior subcapsular) Sight-Threatening |
Contact Dermatitis Infective Conjunctivitis Blepharitis Pemphigoid VKC/SAC/PAC/GPC |
| Vernal Keratoconjunctivitis (VKC) | Some sensitized individuals Peak incidence 3-20 years of age Males predominate 3:1 Bilateral involvement Warm, Dry Climate Seasonal/Perennial Allergens Chronic symptoms |
Severe ocular itching Severe photophobia Thick, ropy discharge Cobblestone papillae Corneal ulceration and scaring Sight-Threatening |
Infective Conjunctivitis Blepharitis AKC/SAC/PAC/GPC |
| Giant Papillary Conjunctivitis (GPC) | Sensitization not necessary Both females and males Bilateral involvement Prosthetic Exposure Occurs Anytime Chronic symptoms |
Mild ocular itching Mild mucoid discharge Giant papillae Contact lens intolerance Foreign body sensation Protein buildup on contact lens Not sight threatening |
Infective Conjunctivitis Preservative Toxicity SAC/PAC/AKC/VKC |
Table 2
Drug and Classification |
Inhibition of Mediator Release From Human Conjunctival Mast Cells |
Inhibitory Effects on Other Cells |
AntazolineH1 Receptor Antagonist |
No Effect | Inhibits IL-6, IL-8 release from on conjunctival epithelial cells in vitro |
PheniramineH1 Receptor Antagonist |
No Effect | Inhibits IL-6, IL-8 release from on conjunctival epithelial cells in vitro |
EmedastineH1 Receptor Antagonist |
No Effect | Inhibits IL-6, IL-8 release from on conjunctival epithelial cells in vitro |
LevocabastineH1 Receptor Antagonist |
No Effect | Inhibits IL-6, IL-8 release, ICAM-1 expression on conjunctival epithelial cells in vitro |
OlopatadineH1 Receptor Antagonist |
histamine, tryptase, PGD2, TNFα in vitro |
Conjunctival mast cell TNFa-mediated upregulation of ICAM-1 on conjunctival epithelial cells in vitro |
KetotifenH1 Receptor Antagonist |
histamine in vitro |
Chemotaxis and activation of eosinophils in vitro |
AzelastineH1 Receptor Antagonist |
in vitro data not available |
Eosinophils and neutrophils in tears ICAM-1 expression in vivo |
CromolynMast cell stabilizer |
not inhibitory for histmaine release in vitro tryptase in tears |
Chemotaxis and activation of eosinophils, neutrophils, monocytes in vitro |
LodoxamideMast cell stabilizer |
in vitro data not available histamine and tryptase in tears |
Chemotaxis and activation of eosinophils in vitro Eosinophils, neutrophils, T cells in tears ICAM-1 expression on conjunctival epithelial cells in vitro |
NedocromilMast cell stabilizer |
not inhibitory for histamine release in vitro |
Activation of eosinophils and neutrophils in vitro |
PemirolastMast cell stabilizer |
not inhibitory for histamine release in vitro |
Activation of eosinophils and neutrophils in vitro |
AntazolineH1 Receptor |
No effect | Inhibits IL-6, IL-8 release from an conjunctival epithelial cells in vitro |
AlcaftadineH1 Receptor |
histamine in vitro | Chemotaxis and activation of eosinophils in vitro |
BepotastineMast Cell stabilizer |
histamine in vitro | Chemotaxis and eosinophils in vitro |