“Learning to perform cataract surgery requires development of highly specialized intraocular microsurgical skills and application of those skills in high-stakes situations with little tolerance for error,” according to Dr. Stephen Sauer, associate professor of comprehensive ophthalmology and cataract surgery curriculum director.
To improve resident acquisition of cataract surgery skills and shift the learning curve into the first year of training, Dr. Sauer and many others developed the new Resident Cataract Surgery Curriculum. Beginning with basic concepts and skills, each program year (PGY) training period builds on progressively more complex didactics, simulation, wet lab and operating room activities.
Multiple faculty provide training and ownership for each faction of the program. It is truly a collaborative effort and many other faculty members also contribute their time and expertise, including senior residents who have an important role for teaching junior residents certain skills and concepts. Dr. Patti Saab, comprehensive ophthalmologist, introduces residents to basic surgical techniques in the wet lab using Kitaro synthetic eye kits and porcine eyes.
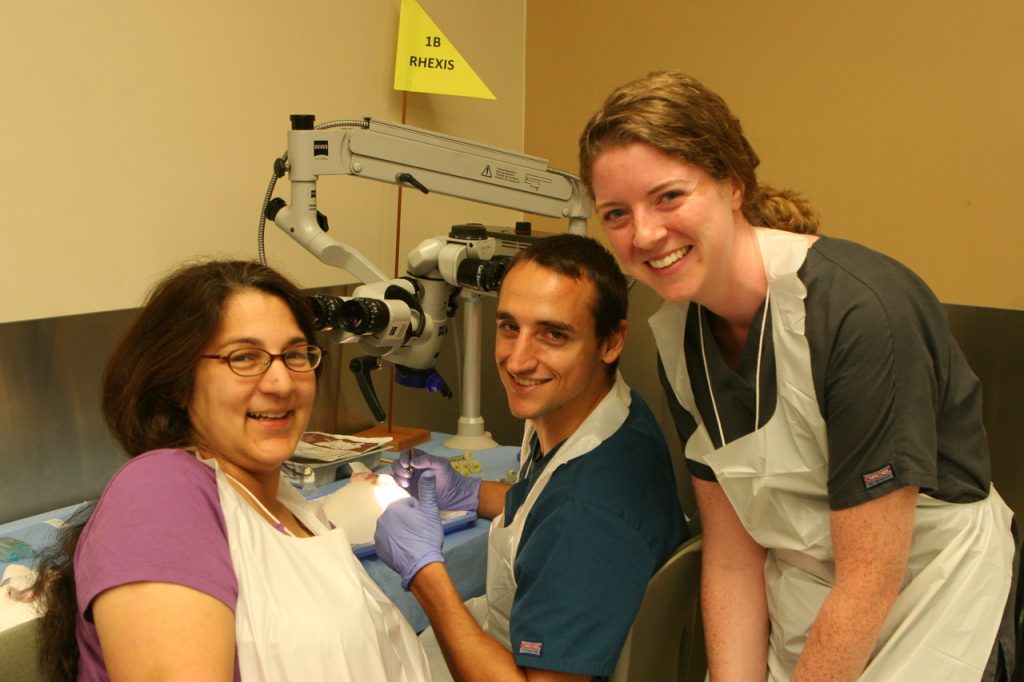
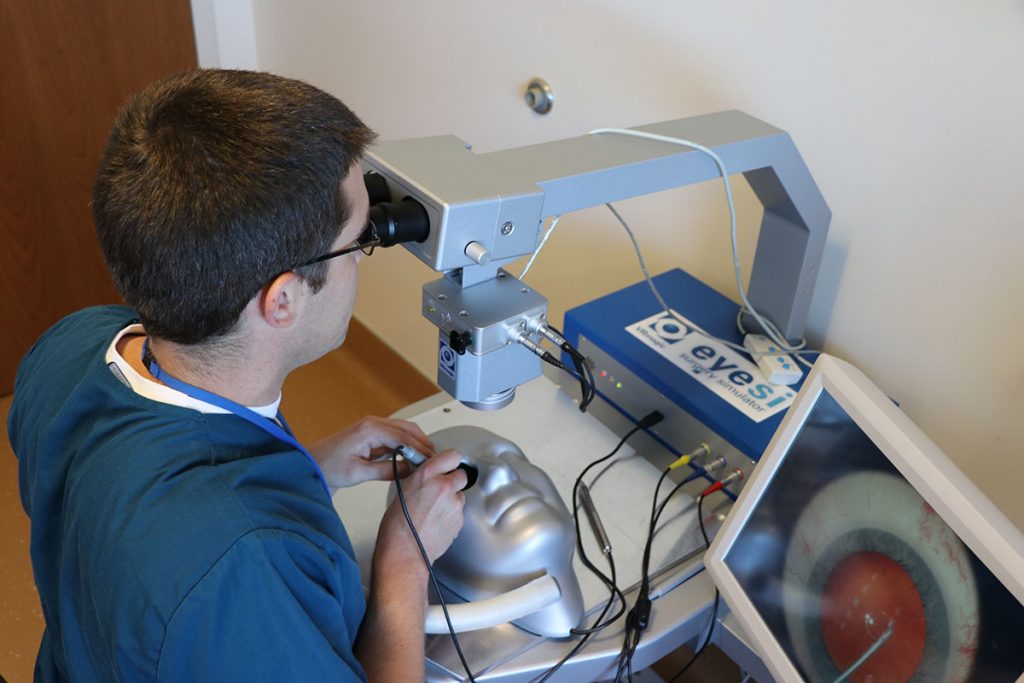
Dr. Yao Liu, glaucoma specialist, provides resident training on the EyeSi surgery simulator (funded and housed at the Veterans Hospital), where residents informally compete for the highest psychomotor skill scores. After practicing specific surgical steps, the new residents are carefully introduced into real cases. Beginning with a lower risk part of a cataract surgery, typically the last step in the procedure, these residents progress using a “back-forward” approach, eventually working through all of the required steps to complete full cases. Each component of the curriculum works together to incrementally develop competency in a particular skill for each step of the surgery. The pace from one step to the next will vary based on the individual trainee, but their efficiency, comfort and rate of successful patient outcomes will increase based on these early and sustained exposures to every facet of the surgical procedure. This enhanced curriculum gives residents ample opportunities to learn more, have hands-on experiences earlier and perfect their techniques in a shortened time frame, all of which develop more apt and ready ophthalmologists of the future.
Currently, each resident must demonstrate cataract surgery competency by performing a minimum of 86 full cataract surgeries before graduation, but most end up with 200 or more. Formerly, the process by which an individual resident achieved that goal began in earnest
during the second (PGY 3) year. Some students with natural ability, or transferable skills learned elsewhere, found the path to becoming skilled in phacoemulsification smooth, but others who seemed to be moving well through other parts of residency training stumbled when they reached cataract surgery. The collaborative development of this new program addresses that gap head-on and has transformed the University of Wisconsin Department of Ophthalmology and Visual Sciences training into a robust, progressive and effective mastering of this common surgical procedure.
“The skills learned from this program will provide the foundation for continuous development of one’s surgical craft even after completing resident training and entering practice,” says Dr. Sauer. “We hope to create an education environment where each resident has access to a similar set of resources, training and surgical opportunities that puts all residents on a smoother path to surgical competence.”
Key Program Features
- Graded and progressive skill acquisition
- Faculty instruction, self-directed practice, periodic assessments
- Didactic knowledge development
- Simulation (EyeSi) psychomotor progressive skills development
- Wet lab psychomotor skills development
- Operating room surgical opportunities, using “back-forward” approach