The American Academy of Ophthalmology recognizes the month of February to promote awareness about Age-related Macular Degeneration, also called simply macular degeneration or AMD, the nation’s leading cause of vision loss. We at the UW Department of Ophthalmology and Visual Sciences want to inform you, our patients and families, about the disease, what to look for if you think you might have AMD and offer insights into how to prevent or stop the progression of macular degeneration, as well as ways to cope with low vision.
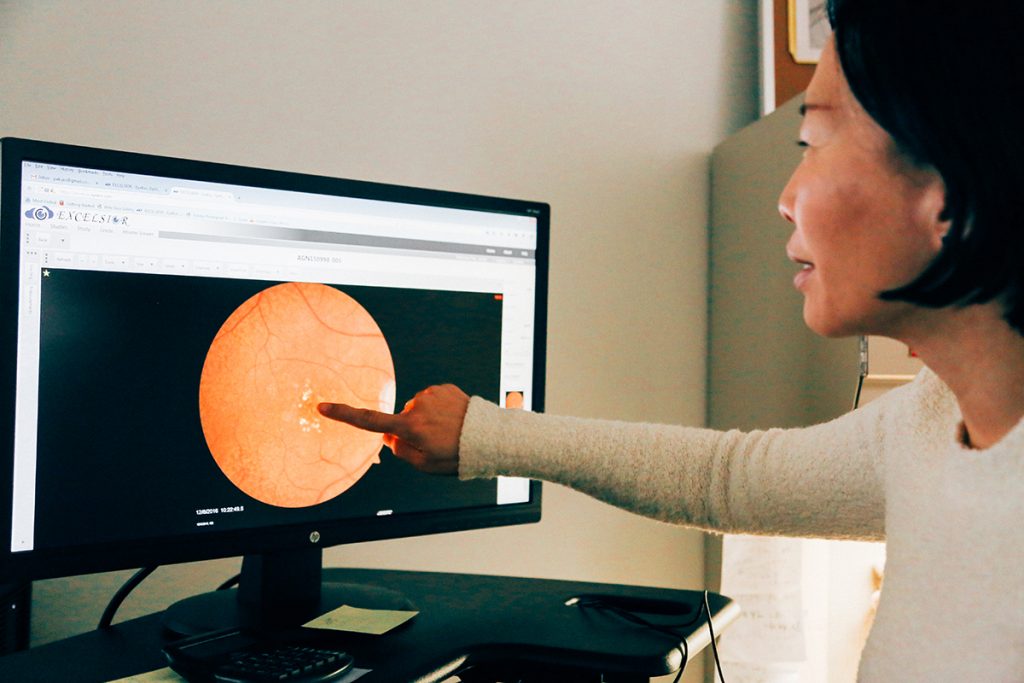
What is age-related macular degeneration?
AMD is a deterioration of the eye’s macula, the central part of the light-sensitive tissue at the back of the eye called the retina. The macula is much more light sensitive than the rest of the retina and helps us focus in fine detail, such as the ability to recognize faces, read fine print, read street signs, etc. As the macula is only a small part of the retina, its degeneration does not usually affect your peripheral vision, which is not as fine and detailed as your central vision.
How does AGE-RELATED macular degeneration occur?
In AMD, as the macular tissue ages, it tends to thin out. Tiny pieces of a fatty protein called drusen start to accumulate under the retina. At some point the macula stops functioning properly and the light signals the retina sends to the brain via the optic nerve become distorted and central vision starts to worsen and may eventually disappear.
Are there different types of AGE-RELATED macular degeneration?
There are two forms of AMD, “dry” and “wet.” The majority of people with macular degeneration have the dry form. With dry AMD, vision loss usually happens more slowly. When dry AMD is diagnosed in early stages your ophthalmologist will see a build-up of medium-sized drusen behind your retina. As the disease progresses and your central vision diminishes, the drusen become larger and there may also be pigment changes in your retina. In late dry AMD the actual light-sensing cells start to break down so they can no longer convey the visual information to the brain. When you are diagnosed with dry AMD, it will be very important to keep a regular appointment with your ophthalmologist because dry AMD can change into the more damaging form called wet macular degeneration. Wet AMD is diagnosed when the doctor sees the growth of abnormal blood vessels underneath the retina. These blood vessels may leak fluid and blood, further distorting your vision. This process can happen faster and cause more noticeable changes than the dry form.
What are the symptoms of AGE-RELATED Macular Degeneration?
The American Academy of Ophthalmology lists the following symptoms for both dry and wet AMD:
Dry AMD:
- Blurry distance and/or reading vision
- Need for increasingly bright light to see up close
- Colors appear less vivid or bright
- Hazy vision
- Difficulty seeing when going from bright light to low light (such as entering a dimly lit room from the bright outdoors)
- Blank or blurry spot in your central vision
One or both eyes can be affected. Often times vision loss in one eye is masked because the other eye compensates, making vision loss virtually unnoticeable.
Wet AMD:
- Distorted vision — straight lines will appear bent, crooked or irregular
- Dark gray spots or blank spots in your vision
- Loss of central vision
- Size of objects may appear different for each eye
- Colors lose their brightness; colors do not look the same for each eye
- Trouble or inability to recognize people’s face
Symptoms of wet AMD typically appear and progress more quickly.
How is AGE-RELATED macular degeneration diagnosed?
The National Eye Institute emphasizes that early and intermediate stages of AMD usually start with no symptoms. The only way to detect AMD is to have a comprehensive eye exam, which may include one of the following:
- Visual acuity test – an eye chart to see how well you can see at a distance and near
- Dilated eye examination – your eye care professional looks inside your eye to inspect the retina for any signs of AMD or other eye problems
- Amsler grid – A visual grid your eye doctor may have you look at to see if there is any distortion or lines missing, a possible sign of AMD
- Fluorescein angiogram – An ophthalmologist will perform this test by injecting a dye into your arm and taking pictures as the dye passes through the eye to gauge any fluid leakage, a possible sign of the wet rapidly, progressive type of AMD
- Optical coherence tomography – a high-resolution test using light waves to image your eyes. The test takes only a few moments and is painless.
During your exam, your doctor will be looking for evidence of drusen deposits underneath your retina. The presence of larger deposits is indicative of AMD. Your doctor will also be looking for possible changes in your eye pigment underneath your retina with development of areas of dark pigment clumping and other areas of loss of pigment. This is another possible sign of AMD.
facts about AGE-RELATED MACULAR DEGENERATION:
- According to the American Macular Degeneration Foundation, AMD affects more than ten million Americans, more than cataracts and glaucoma combined.
- AMD is the leading cause of vision loss among people over 50. The disease usually affects people who are 60+, but it can occur earlier.
- Age is the major risk factor for AMD. Other risk factors include smoking and people with a family history of AMD.
- People of Caucasian descent are more likely to develop AMD than those of African American or Hispanic/Latino descent.
- AMD does not lead to complete blindness, only affecting your finest central vision. AMD usually does not impact your peripheral vision. People with advanced AMD may develop legal blindness due to loss of central vision.
- There is no cure for AMD, only treatments that can help slow its progression.
- AMD usually affects both eyes, but one eye may be affected before the second eye.
- Many people do not know they have AMD until they have a noticeable vision problem, or until it is discovered during a routine eye examination.
- There are two kinds of AMD, “wet” and “dry.”
- Early detection is key to slowing the progression of AMD.
SOURCE: National Eye Institute, American Academy of Ophthalmology, American Macular Degeneration Foundation.