A current clinical trial in the UW Department of Ophthalmology and Visual Sciences Clinical Eye Research Unit (CERU) could lead to approval of a first-ever treatment option for patients with geographic atrophy (GA) secondary to age-related macular degeneration, a progressive, irreversible, and devastating eye disease.
GA is a progressive condition and is the leading cause of blindness in patients over age 65 in developed nations. It affects 5 million people worldwide, including more than 1 million in the United States.
Patients with geographic atrophy develop visual impairment due to the loss of photoreceptor cells in the macula – the central portion of the retina that provides central vision and color perception. Small areas of damage in the early stages gradually grow into larger patches of GA (lesions) as the disease progresses, resulting in permanent blind spots that affect anything from reading to driving to recognizing people’s faces.
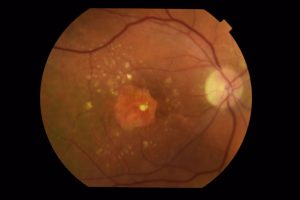
While this condition is responsible for 20% of all cases of legal blindness in North America, there is currently no treatment available. However, results from a recent clinical trial may change that.
CERU researchers have participated in a multi-center study sponsored by Apellis Pharmaceuticals that evaluated the long-term safety and effectiveness of a new investigational product, pegcetacoplan.

“This new therapeutic agent targets an important pathway involved in the development of GA and has showed promising results by slowing down the growth rate of these lesions,” said Mihai Mititelu, MD, MPH, FASRS, principal investigator of the trial at UW and medical director of the Clinical Eye Research Unit.
The clinical trial involved the injection of the medication directly into the vitreous cavity – a gel-filled compartment in the back of the eye. Study participants received either a placebo or the pegcetacoplan injection every 4 or 8 weeks for a total of 24 months.
“Both monthly and every-other month study arms demonstrated reduction in GA lesion growth and had a favorable safety profile,” said Dr. Mititelu.
Pegcetacoplan is currently under review by the Food and Drug Administration, with a decision expected to be announced in February 2023. “If approved,” Dr. Mititelu added, “this potential therapeutic agent could be an important move in the right direction for GA patients who currently have no treatment options for their relentless condition.”
From a clinician’s perspective, Dr. Mititelu emphasized the importance of applying study results to everyday clinical practice by tailoring new therapies such as pegcetacoplan to individual patient circumstances. “This new agent will hopefully become the first tool in the growing armamentarium that addresses one of retina’s most significant unmet therapeutic needs,” he said.